INTRO: The current data on coronavirus infection and mortality rate has shown that the unequal burden for life among people of race and ethnicity is 100% real and an extremely diverse human society aiding the pandemic scourge strives in Florida. Excerpt.
That the black Americans are now more likely unsafe is a fact the deadly coronavirus pandemic has scaled up by 59% in Florida. This is at a time when the white Americans are 41% safer from being killed by the virus.
The data obtained over the weekend about the state from Covid-19 Tracking Project on Infection and Mortality by Race and Ethnicity showed people of color risk coronavirus complications more and disproportionately die than the rates for the white people appears not not unnoticed by people in the state.
“There is no clinical evidence that people of color have genetic or other biological factors that make them more likely to be affected by the deadly coronavirus pandemic,” saidWilliam Marshfield, a public health practitioner.
He fielded questions on why people of color get sick and die at disproportionate rates in Florida.
“They are more likely to have underlying health conditions,” he explained.
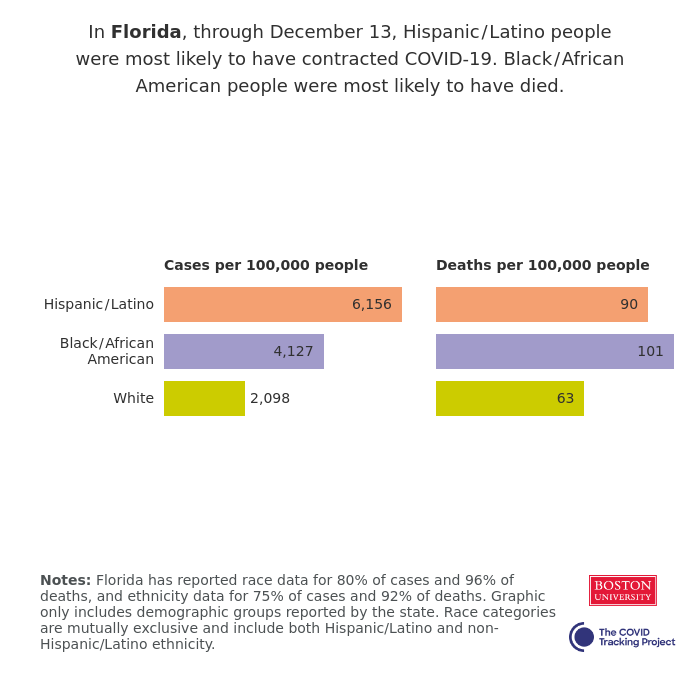
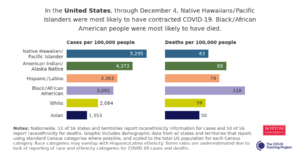
More updates on the Covid Tracking Project has also shown that while Hispanic/Latino people are more likely to have contracted the virus compared with other races, Black Americans are more likely to have died of COVID-19 in the state.
Covid Tracking Project, a reputable and independent research group, also revealed a likelihood of 5,138 cases per 100,000 Latino people in the state with a death case of 82 per 100,000 thousand among the group of people.
The dataset, which is often updated every two weeks, also revealed that 97 people die out of every 100,000 Black folks with covid infection. It also warned about the possibility of 3,840 cases of COVID-19 among every 100,000 individuals among the group of people.
In Florida, out of every 100,000 white people with the virus, unfortunately 59 people may not survive it. The number of deaths is 41% less than the percentage rate at which black people die of the same infection in the same state.
“Those numbers are scaled by how many numbers of each group live in the state,” Alice Goldfarb, CRDT Lead at Covid-19 Tracking Project confirmed in a chat.
As at the time of filing this report, the Covid Tracking Project data indicated that Florida has reported race data for 79% of cases and 96% for deaths, and it also has ethnicity data for 74% of cases and 92% of deaths through the first week of December.
“Having certain conditions, such as type 2 diabetes, increases your risk of severe illness with covid-19.”
Marshfield, the public health practitioner, has emphasized that where people live and work affects their health. And over time, these factors lead to different health risks among racial and ethnic minority groups.
“Where you live and who you live with can make it challenging to avoid getting sick with COVID-19 and be able to get treatment. For example, racial and ethnic minority members might be more likely to live in multi-generational homes, crowded conditions and densely populated areas, such as some part of Brooklyn in New York City and somewhere like Palatka in Florida and this can make social distancing difficult,” he said.
Palatka, unfortunately, ranks as the poorest place in Florida thanks to a combination of low pay and a lack of jobs. The city of 10,291 people averages the 1st lowest median household income in Florida and the first highest in poverty rate.
“More worrisome is the type of work most of the hardworking minorities do.” Marshfield said, stating that this also may contribute to balck/Africans risk of getting covid-19 than the white people who do most of their work in the confine of their safe and comfort zones.
“Many people of color have jobs that are considered essential or can’t be done remotely and involve interaction with the public. According to the Centre for Disease Control(CDC) nearly 25% of employed Hispanic and Black or African Americans work in the service industry, compared with 16% of non-Hispanic white workers.
“Black or African Americans also account for 30% of licensed practical and licensed vocational nurses. Many people of color also depend on public transportation to get to work. These factors can result in exposure to the virus,” he further explained.
Speaking further Marshfield noted that lack of access to health care is rampant among members of racial and ethnic minority groups and that this is not just common in Florida but likely in every other states in America.
He noted that the black Americans are more likely to encounter barriers to get access for health care, such as health insurance explaining that qualitative health care should right for all as every individuals would need to keep healthy status to guard against being covid19 sick.
According to the Centre for Disease Control only about 6% of non-Hispanic white people were uninsured, while the rate was nearly 18% for Hispanics and 10% for non-Hispanic black people.
Marshfield was of the view that racism may also play a role on health risks of the black communities stating that the stress of dealing with racial discrimination can take a toll on your body, causing early aging. “And this is a proof link to underlying conditions, which can increase the risk of severe illness with coronavirus.
“All of these factors — underlying health conditions, dense living conditions, employment in the service industry or as an essential worker, access to health care and racism — contribute to the impact of covid-19 on people of color.”
“But these are long-standing issues,” he added.